Home » Articles » What to Know About the WHO-Recommended Malaria Vaccine
October 8, 2021
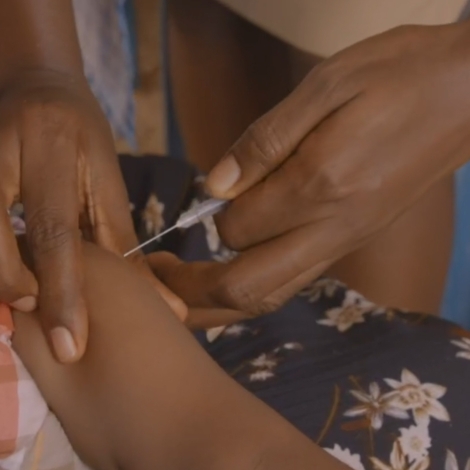
What to Know About the WHO-Recommended Malaria Vaccine
Please sign-up or login
Not a member? Sign Up
Suggested Articles
Do you have a video game on pause while you’re reading this? If so, you have lots of company. There may be 500 million people worldwide who play...
Read Full Article